The “Hip Kit” Explained: 5 Tools You Need After Hip Replacement Surgery
After surgery, your doctor or physical therapist will likely give you a strict rule: The 90-Degree Rule. You must not bend your hip past a 90-degree angle, cross your legs, or twist your hip inward. This precaution is vital to prevent your new hip joint from dislocating while it heals.
But if you can’t bend past 90 degrees, how do you put on your socks? How do you pick up the remote control you dropped? How do you wash your feet?
Enter the “Hip Kit.”
Here is a breakdown of the 5 essential tools found in a standard Hip Kit and why you can’t recover without them.
1. The Reacher Grabber

The MVP (Most Valuable Player) of your recovery will undoubtedly be the reacher. This is a lightweight pole with a handle at one end and a mechanical jaw at the other.
- Why you need it: Bending over to pick up objects from the floor is the #1 way patients accidentally break the 90-degree rule.
- How to use it: Use it to pick up dropped items, reach books on low shelves, or even pull your pants up to your knees before you stand.
- Tip: Many of our clients buy two—one for the bedroom and one for the living room/kitchen—so they never have to walk around looking for it.
2. The Sock Aid
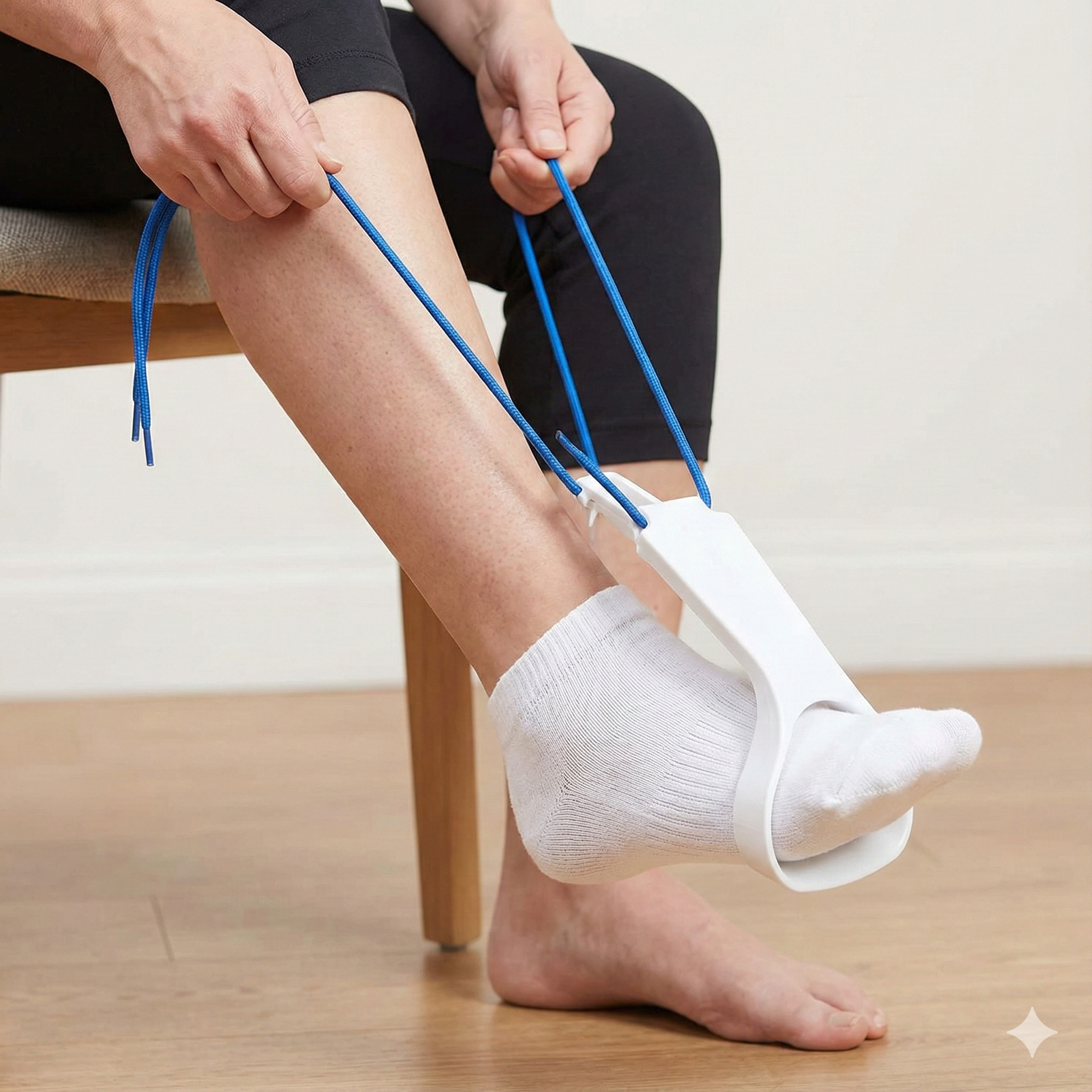
Ask anyone who has had hip surgery what their biggest frustration is, and they will likely say, “Putting on socks.” It is physically impossible to put on a sock without bending your hip too far unless you have help or the right tool.
- Why you need it: Independence. You don’t want to have to call a caregiver every time your feet get cold.
- How it works: The reacher grabber sock aid combo is often talked about, but the sock aid is a specific device. You slide your sock over a flexible plastic tube attached to long cords. You drop the tube to the floor (holding the cords), slide your foot in, and pull. The sock slides perfectly onto your foot without you bending an inch.
3. Long-Handled Shoe Horn
Once your socks are on, you need shoes. Sturdy, non-slip shoes are crucial for learning to walk again, but jamming your heel into a sneaker requires force and bending.
- Why you need it: To protect your heels and your new hip. A standard shoe horn is too short. A long-handled version (usually 18-24 inches) allows you to guide your foot into the shoe while standing upright or sitting safely.
4. Long-Handled Bath Sponge

Hygiene is important for preventing infection and feeling like yourself again. However, reaching your lower legs, feet, and back in the shower can be dangerous on a slippery surface.
- Why you need it: Safety in the shower.
- How to use it: These sponges are mounted on a long, often curved handle. They allow you to scrub your feet and back without twisting your torso or bending down, significantly reducing the risk of a slip-and-fall accident in the bathroom.
5. The Dressing Stick

This looks like a simple wooden dowel with hooks on both ends, but it is a versatile tool for getting dressed.
- Why you need it: Dressing your lower body is tricky.
- How to use it: The hooks help you pull up trousers, straighten skirts, or push down socks that are bunched up. It acts as an extension of your arm, handling the fabrics that are just out of reach.
Why Buy a Kit Instead of Separate Items?
While you can purchase these items individually, buying a pre-packaged “Hip Kit” from a medical supply provider like Alfa Healthcare Supply Inc. is usually more cost-effective. Furthermore, these kits are curated by experts who know exactly what quality of hip replacement recovery equipment is required for daily hospital-grade use.
Recovery Tip: Practice using these tools before your surgery. It takes a little coordination to master the sock aid or the reacher. If you practice while you are mobile, you will be a pro by the time you get home from the hospital.
Understanding Home Oxygen Support Systems: A Guide for Recovery
For many patients, recovery doesn’t stop when they leave the hospital—especially when breathing support is part of the journey. Home oxygen therapy can make a world of difference by improving energy, reducing strain on the heart, and helping your body heal faster.
If your doctor recommends oxygen support at home, here’s everything you need to know about choosing, using, and maintaining the right home oxygen support system safely.
If you’re preparing for discharge, make sure you check out our guide on Patient Discharge Checklist: Essential Home Recovery Equipment to plan your complete recovery setup.
1. What Is Home Oxygen Therapy?
Home oxygen therapy provides extra oxygen to people who have trouble maintaining adequate blood oxygen levels. It’s commonly used for:
- Post-surgery recovery
- Chronic respiratory issues
- COVID-19 or pneumonia recovery
- COPD and sleep apnea management
Supplemental oxygen helps your body function better and prevents fatigue, confusion, or shortness of breath during recovery.
2. Types of Home Oxygen Support Systems
Choosing the right oxygen system depends on your doctor’s prescription and your mobility needs. Here are the most common options:
Oxygen Concentrator
This machine draws in room air and filters out nitrogen, delivering pure oxygen through a nasal cannula.
- Ideal for home use
- Continuous oxygen flow
- Low maintenance and cost-effective
Portable Oxygen Concentrator (POC)
Lightweight and travel-friendly, POCs are perfect for patients who want mobility and independence.
- Battery-operated
- Pulse flow delivery (oxygen when you inhale)
- Great for errands or appointments
Oxygen Cylinders
Cylinders contain compressed oxygen and are often used as backup for emergencies or short-term recovery.
- Available in multiple sizes
- Easy to replace/refill
- Must be stored upright and handled carefully
3. Nebulizers and Humidifiers
Some patients may also need nebulizers to deliver medication directly to the lungs or humidifiers to add moisture to oxygen flow—especially if dryness causes discomfort.
Tip: Always clean nebulizer cups and tubing after every use to prevent infections.
4. Setting Up Home Oxygen Safely
A safe home setup ensures both comfort and peace of mind:
- Place the concentrator in a well-ventilated area
- Keep oxygen equipment away from open flames or heat sources
- Avoid using petroleum-based products on your face or near oxygen flow
- Never smoke around oxygen—it’s highly flammable
Pro Tip: Have backup power or extra cylinders ready in case of a power outage.
5. Monitoring Oxygen Levels
Use a pulse oximeter to track your oxygen saturation (SpO₂) regularly.
- Normal range: 95%–100%
- Contact your healthcare provider if it drops below 90%
Keeping a daily log helps your doctor adjust flow rates if needed.
6. Maintenance and Servicing
Just like any medical equipment, regular maintenance ensures safety and performance:
- Clean filters weekly
- Replace nasal cannulas every 2–3 weeks
- Schedule annual servicing for concentrators
Cleanliness and upkeep can extend your equipment’s lifespan and prevent breathing issues.
7. Rent or Buy? Choosing What Works for You
If oxygen therapy is temporary, renting a concentrator or cylinder may be cost-effective. For long-term needs, purchasing your own unit can offer more convenience.
Still unsure? Our Patient Discharge Checklist blog covers detailed tips on rent vs. buy decisions for home care equipment.
Conclusion: Breathe Easy, Recover Confidently
Home oxygen support systems are life-enhancing tools that bring hospital-quality care into your home. When used correctly, they can help you recover comfortably, maintain your independence, and breathe better every day.
Remember—a well-prepared home is a healing home.
Serving New York, Queens, Long Island, Brooklyn, Bronx, and Westchester with reliable medical supplies and durable healthcare equipment.
How to Use a Nebulizer Correctly – A Beginner’s Guide
For people living with respiratory conditions such as asthma, COPD, or chronic bronchitis, a nebulizer can be a lifesaver. It converts liquid medication into a fine mist that is inhaled directly into the lungs, providing fast and effective relief.
For step-by-step instructions on long-term upkeep of devices, you may also want to read our caregiver’s guide to cleaning medical equipment, which explains best practices for sanitizing and maintaining all types of home healthcare supplies.
What Is a Nebulizer?
A nebulizer is a small machine that turns liquid medicine into a breathable mist. Unlike inhalers, which require coordination and strong inhalation, nebulizers are easier for children, elderly patients, and anyone struggling with severe breathing difficulties.
There are different types:
- Jet Nebulizers – Most common, powered by compressed air.
- Ultrasonic Nebulizers – Use high-frequency vibrations to create mist.
- Mesh Nebulizers – Portable, battery-powered, and quieter.
When Is a Nebulizer Needed?
Doctors often prescribe nebulizers for:
- Asthma flare-ups
- COPD management
- Cystic fibrosis treatment
- Respiratory infections needing inhaled antibiotics
- Severe allergies causing breathing problems
In the future, many nebulizers will be integrated with smart medical devices, allowing doctors to monitor usage remotely.
Mistakes to Avoid
- Not cleaning after use – This allows bacteria and mold to grow.
- Incorrect posture – Slouching reduces medicine delivery.
- Rushing the process – Inhaling too fast may not deliver full dosage.
- Skipping replacement parts – Tubing and filters wear out over time.
Maintenance & Replacement Schedule
- Tubing: Replace every 6 months.
- Mouthpiece/Mask: Replace every 3–6 months.
- Filter: Check monthly, replace if discolored.
- Compressor: Service annually or as recommended.
Many new nebulizers now come with digital sensors and app tracking. Our guide on smart medical devices in home healthcare explores how technology is transforming respiratory care.
Safety Precautions
- Always use medication prescribed by your doctor.
- Store medicines in a cool, dry place.
- Never self-adjust dosages without medical advice.
- If your machine stops working, avoid DIY electrical fixes—contact the supplier.
Tips for Caregivers
- Encourage patients to stay calm and breathe normally.
- Use distraction for children (reading, cartoons).
- Keep a written log of treatment times and doses.
- Make cleaning part of the daily routine.
For more caregiver support, see our equipment maintenance guide, which includes a printable cleaning checklist.
Conclusion
Using a nebulizer correctly ensures that patients get the full benefit of their medication. By following proper setup, cleaning, and maintenance steps, you can keep the device safe and effective for years.
Want to know what’s next in respiratory care?
Read our article on the role of smart medical devices in home healthcare to see how technology is making treatment more efficient and personalized.
Air Quality and Health: How a Humidifier or Nebulizer Can Help You Breathe Easier
The air we breathe has a significant impact on our respiratory health. From dry indoor air that irritates the throat and sinuses to environmental allergens that trigger asthma, air quality is a key concern. Fortunately, with the right Durable Medical Equipment (DME), you can create a healthier, more breathable environment right in your own home. A humidifier or nebulizer can be a game-changer for those seeking to breathe easier.
The Power of a Humidifier
A humidifier adds moisture to the air. This is especially beneficial in dry climates or during winter when indoor heating systems can strip the air of its natural humidity.
- Relieves Sinus Congestion: Moist air can help thin mucus and make it easier to clear congestion.
- Soothes Sore Throats: It can alleviate the dryness and discomfort of a sore throat or cough.
- Hydrates Skin: A humidifier can also prevent dry, itchy skin and chapped lips.
The Targeted Relief of a Nebulizer
A nebulizer is a medical device that turns liquid medicine into a fine mist that can be inhaled directly into the lungs.
- Delivers Medication Effectively: For individuals with asthma, COPD, or other respiratory conditions, a nebulizer ensures that the medication reaches the lungs directly and quickly.
- Treats Respiratory Flare-Ups: During an asthma attack or a severe cough, using a nebulizer can provide fast and effective relief.
Conclusion :
Whether you need to add moisture to the air with a humidifier or deliver targeted medication with a nebulizer, these devices can significantly improve air quality and health at home. By understanding the purpose of each, you can make an informed choice to help you and your family breathe easier, every day.
Taking Your Respiratory Therapy Equipment on the Go: A Guide to Traveling with a Nebulizer
If you rely on a nebulizer for your respiratory therapy, the thought of traveling can be daunting. But with the right preparation and a few simple tips, you can take your respiratory therapy equipment with you wherever you go, ensuring you stay healthy and comfortable away from home. This guide will help you pack smart and travel stress-free with your nebulizer.
Step 1 : Get Your Supplies and Documents in Order
Before you pack, make sure you have everything you need.
- Medication: Bring enough medication for your entire trip, plus a little extra in case of delays. Keep all medications in their original, clearly labeled containers.
- Prescription: Carry a copy of your prescription for your nebulizer and all medications. This is crucial, especially for international travel, to avoid any issues at airport security.
- Doctor’s Letter: A letter from your doctor explaining your condition and the necessity of your respiratory therapy equipment can be very helpful.
Step 2 : Packing Your Nebulizer
- Carry-On is Key: Always pack your nebulizer in your carry-on bag. This prevents it from getting lost, damaged, or exposed to extreme temperatures in the cargo hold.
- Organize Your Nebulizer Kit: Use a small, separate bag or carrying case to keep all your nebulizer kit components together, including the machine, tubing, mouthpiece, and face mask.
- Batteries: If you have a battery-operated nebulizer, check the airline’s regulations on carrying batteries. If you plan to use it on the plane, ensure the batteries are fully charged and carry a backup if needed.
Step 3 : Navigating Airport Security and Travel
- Declare Your Equipment: When you go through security, inform the TSA or airport security agent that you have medical equipment.
- Air Travel: Most airlines allow medical equipment, like a nebulizer, to be carried on and used during a flight. However, it’s always best to check with your airline beforehand to confirm their specific policies.
- Hotel Stays: Remember to pack a converter and/or adapter if you’re traveling internationally, as power outlets and voltage can vary.
Conclusion
Don’t let your respiratory therapy equipment hold you back from traveling. By preparing in advance and packing your nebulizer correctly, you can ensure you have the peace of mind that comes with knowing your health is a top priority, no matter where your journey takes you.
Understanding Your BIPAP Machine: How It Works and When It’s Recommended
For many people with sleep apnea, a CPAP machine is the go-to solution. However, for some, a BIPAP machine (Bilevel Positive Airway Pressure) is a more effective form of respiratory therapy equipment. While they may look similar, a BIPAP machine works differently and can be a game-changer for people who can’t tolerate traditional CPAP therapy. This guide will help you understand the core differences and when a BIPAP machine might be the right choice for you.
How a BIPAP Machine Works
The primary difference between a CPAP and a BiPAP machine lies in the pressure they deliver. A CPAP machine delivers a single, constant air pressure throughout the night. A BIPAP machine provides two distinct pressure levels:
Type 1 Diabetes: An Autoimmune Condition
- Inspiratory Positive Airway Pressure (IPAP): A higher pressure when you inhale.
- Expiratory Positive Airway Pressure (EPAP): A lower pressure when you exhale.
This difference in pressure makes breathing out against the machine’s airflow much easier and more comfortable, which is a major benefit for many users.
When is a BIPAP Machine Recommended?
A BIPAP machine is often recommended by a doctor when a person:
- Struggles with CPAP Intolerance: Many people find it difficult to exhale against the continuous pressure of a CPAP machine. The lower pressure during exhalation with a BiPAP machine can make the therapy more comfortable and encourage compliance.
- Has Central Sleep Apnea: While a CPAP machine is effective for Obstructive Sleep Apnea, a BiPAP machine can be more helpful for Central Sleep Apnea, where the brain fails to signal the muscles to breathe.
- Has Other Conditions: A BIPAP machine is often prescribed for people with other respiratory conditions, such as COPD (Chronic Obstructive Pulmonary Disease), where breathing is already difficult.
Advantages of a BIPAP Machine
Home Management of Type 1 Diabetes Home management for Type 1 diabetes is non-negotiable and revolves entirely around replacing the insulin the body can no longer produce. Key components include:
- Enhanced Comfort: The ability to exhale against a lower pressure makes it easier to breathe naturally.
- Improved Compliance: Because it’s more comfortable, patients are more likely to use their therapy consistently, which is key to its success.
- Better Therapy for Specific Conditions: The dual-pressure delivery is tailored to meet the needs of people with specific breathing disorders beyond standard sleep apnea.
Conclusion
While a CPAP machine is a highly effective treatment for most people with sleep apnea, a BIPAP machine provides a valuable alternative for those who need a more comfortable or advanced form of respiratory therapy equipment. Discussing your specific needs with your doctor is the best way to determine if a BIPAP machine is the right choice to improve your sleep and overall health.
The Ultimate Guide to CPAP Headgear: Finding the Perfect Fit for Your Sleep
For successful sleep apnea therapy, the fit of your mask is everything. The most critical component of that fit is your CPAP headgear. Finding the right one can mean the difference between waking up refreshed and struggling with leaks, discomfort, and skin irritation. This guide will walk you through how to choose and adjust your CPAP headgear for the perfect fit and a better night’s sleep.
Why a Proper Headgear Fit Matters
The CPAP headgear is designed to hold your mask in place to create a seal and maintain the correct air pressure. If it’s too loose, the mask will leak, reducing the effectiveness of your therapy. If it’s too tight, it can cause red marks, sores, and discomfort, making it difficult to fall and stay asleep. A good fit is a balance of stability and comfort.
Choosing the Right Type of Headgear
There are a few different styles of CPAP headgear, and each has its own benefits:
- Standard Headgear: Most masks come with this type, which has four straps (two on top, two on bottom) that meet at the back of the head. It’s highly adjustable and offers a secure fit.
- Minimalist Headgear: Some designs feature fewer straps or a more streamlined profile. This can be more comfortable for people who feel claustrophobic or for those who sleep on their side.
- Full-Head Headgear: This style is often used with a full face mask for a more secure fit, as it distributes pressure over a larger area.
Tips for Adjusting Your CPAP Headgear for a Perfect Fit
- Don’t Over-Tighten: This is the most common mistake. Start by loosening all the straps, then gently tighten them, one at a time, until the mask feels snug. The goal is to create a seal, not to clamp the mask to your face.
- Adjust While Lying Down: The shape of your face changes when you lie down. Adjust your CPAP headgear while you are in your normal sleeping position to get the most accurate fit.
- Check for Leaks: With the machine running, feel around the edges of the mask to check for air leaks. If you find one, adjust the nearest strap just enough to stop it.
- Use It Consistently: It may take a few nights for your CPAP headgear to feel comfortable. Wear it every night to allow your skin to adjust to the sensation.
Conclusion
Finding the perfect fit for your CPAP headgear is a journey, but it’s one that is worth the effort. A comfortable, secure fit can make all the difference in the quality of your sleep therapy.
Nebulizer vs. Inhaler: How to Choose the Right Respiratory Therapy Equipment for Your Needs
When managing a respiratory condition, medication delivery is a key part of your treatment. Two of the most common devices are nebulizers and inhalers, but they are not the same. Understanding the differences between a nebulizer and an inhaler is the first step to choosing the right respiratory therapy equipment for you or a loved one. This guide will help clarify their functions so you can have an informed discussion with your doctor.
Important Disclaimer: Always consult with a healthcare professional to determine which device is right for your specific condition.
Understanding the Nebulizer
A nebulizer is a machine that turns liquid medication into a fine mist. This mist is then inhaled through a mask or a mouthpiece, allowing the medicine to be delivered deep into the lungs.
- Best For: A nebulizer is often recommended for young children, infants, or older adults who may have difficulty using an inhaler. It is also a good choice for people with severe asthma attacks or other conditions that make deep breathing difficult.
- Pros: Requires no special breathing technique; delivers medication over a longer period (usually 10-15 minutes); very effective for severe symptoms.
- Cons: Not portable (usually requires a power source); takes a longer time to administer medication.
Understanding the Inhaler
An inhaler is a small, portable device that delivers a puff of medication directly into the lungs. There are two main types: Metered-Dose Inhalers (MDIs) and Dry Powder Inhalers (DPIs).
- Best For: Inhalers are commonly used for managing mild to moderate asthma and COPD. Their portability makes them ideal for quick relief on the go.
- Pros: Highly portable and compact; quick and easy to use.
- Cons: Requires a specific breathing technique to be effective; can be difficult for some people to use correctly.
Nebulizer vs. Inhaler: How to Choose
The choice between a nebulizer and an inhaler depends on your age, physical ability, and the severity of your condition.
- Consider a Nebulizer if: You need a high dose of medication, you have trouble coordinating your breathing with an inhaler, or you have a severe flare-up.
- Consider an Inhaler if: You need a quick, portable solution for daily management and are able to use it with the correct technique.
For many, a combination of both is the ideal solution—an inhaler for daily use and a nebulizer for home use during severe episodes.
Conclusion
Both a nebulizer and an inhaler are vital tools in respiratory therapy equipment. The key is to discuss your needs with your doctor to determine which one will be most effective for you. Having the right device can make a significant difference in managing your condition and improving your quality of life.
Troubleshooting Your CPAP Machine: A Guide to Common Issues and Solutions
A CPAP machine is a life-changing device for people with sleep apnea, but like any piece of equipment, it can run into a few issues. When your machine isn’t working as it should, it can be frustrating and disrupt your sleep therapy. This guide will help you troubleshoot some of the most common problems with your CPAP machine and provide simple solutions to get you back to a good night’s rest.
Important Disclaimer: If you continue to have issues with your CPAP machine or your therapy, contact your equipment provider or doctor.
Problem 1 : Mask Leaks
This is one of the most common issues with a CPAP machine. A mask leak can reduce the effectiveness of your therapy and cause dry eyes and skin irritation.
- Solution: Check the fit of your mask. Your CPAP headgear should be snug but not too tight. Over-tightening can actually cause more leaks. Try to adjust the straps while lying down in your usual sleeping position. Ensure your nasal mask cushion or seal is clean and free of oils from your skin.
Problem 2 : Nasal and Throat Dryness
Waking up with a dry mouth, nose, or throat can be very uncomfortable.
- Solution: Use a heated humidifier for CPAP if you aren’t already. This device adds moisture to the air you’re breathing. If you are using one, check the water level and ensure the humidifier is on. You may also need to increase the humidity setting. Using a heated tubing can also help, as it prevents condensation and ensures the air remains warm and moist.
Problem 3 : The Machine is Too Loud
While modern CPAP machines are very quiet, sometimes a new or sudden noise can be a sign of a problem.
- Solution: First, check the air filter. A clogged filter can make the motor work harder and become louder. Replace your disposable filter regularly. Also, inspect your CPAP tubing for any small leaks or tears.
Problem 4 : The Pressure Feels Too High or Too Low
The pressure from the machine can feel uncomfortable or insufficient for your needs.
- Solution: Do not adjust the pressure settings on your own. This should only be done by a healthcare professional. Discuss your concerns with your doctor. They may recommend a ramp feature that starts with a lower pressure and gradually increases, or they may adjust your prescription to a more comfortable level.
Conclusion
While troubleshooting your CPAP machine can be frustrating, most issues have a simple solution. Regular cleaning, proper mask fitting, and utilizing accessories like a heated humidifier for CPAP can solve most problems. By staying on top of your machine’s maintenance, you can ensure your sleep apnea therapy remains effective and comfortable.